Rupali Lal
Bachelor of Pharmacy (Hons), Functional Nutritional Therapy Practitioner, Pause Breathwork Facilitator, Restorative Wellness Practitioner, RESTART® instructor
In part 1, we explored the effects of slow breathing on the brain, cardiovascular, respiratory, and gastrointestinal systems, as well as its influence on mental health. In this section, we will delve deeper into how slow breathing impacts:
- Pain management
- Immunity
- Sleep
- Physical performance
- Blood glucose regulation
Pain management
Research shows that slow deep breathing (SDB) can help reduce the intensity of pain.
One study found that pain intensity decreased when people practiced slow breathing with longer exhalations compared to inhalations (i.e., a low inspiration-to-expiration ratio).[1]
In this study, 48 healthy participants rated their pain after being exposed to heat at three different intensities while using four different breathing patterns.
The results showed that the most intense heat was rated as less painful when participants used a slow breathing technique with a longer exhale with a 20% reduction in pain compared to unpaced breathing at highest heat intensity.
Overall, the study demonstrated that slow-paced breathing can reduce pain perception, with the effect being more pronounced when breathing is paced at a lower frequency (six breaths per minute) and includes a low inspiration-to-expiration ratio.
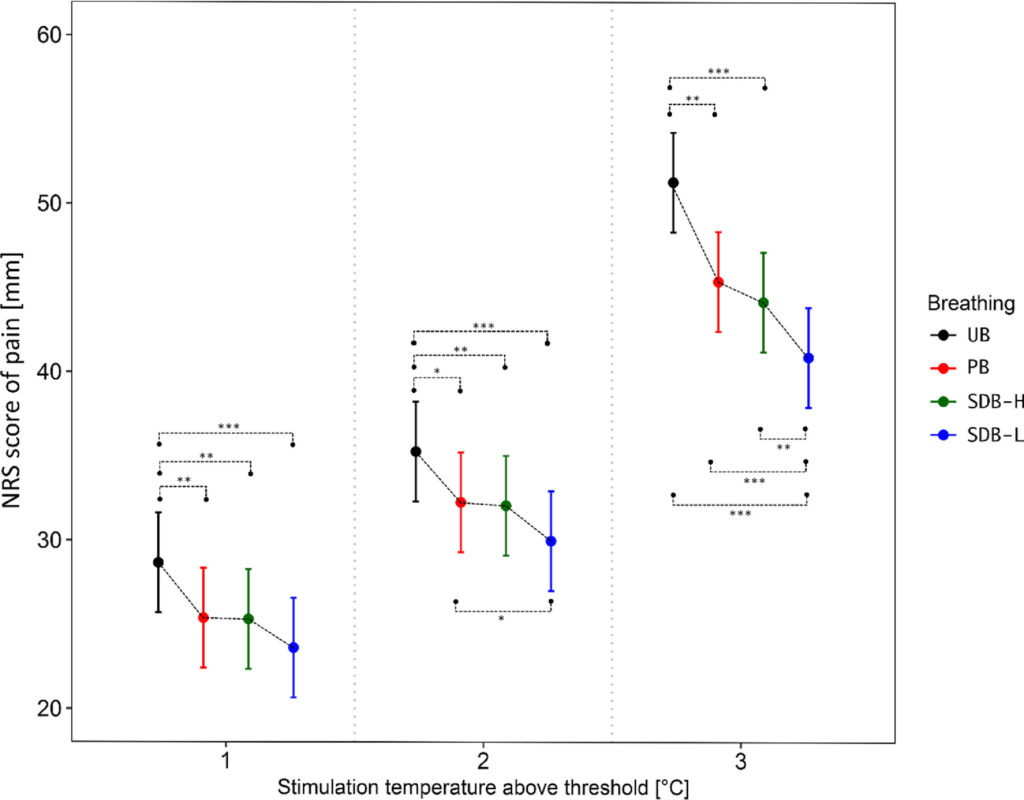
Abbreviations: NRS, numeric rating scale; mm, millimeter; UB, unpaced breathing; PB, paced breathing; SDB-L, slow deep breathing with low inspiration/expiration ratio; SDB-H, slow deep breathing with high inspiration/expiration ratio.
Another study looked at how Slow Deep Breathing Relaxation Exercise (SDBRE) helped patients during removal of chest tubes after heart surgery. Out of 50 patients, 25 practiced SDBRE before the procedure along with standard care, while the other half received standard care only.[2]
Slow-paced breathing can reduce pain perception
Pain levels were measured:
- before the removal
- 5 minutes after the removal
- 15 minutes after the removal
The group using slow breathing showed a dramatic reduction in pain — almost a 100% decrease by the final measurement compared to 50% in the control group.
Lastly, an evidence-based breathing protocol was developed specifically for managing chronic pain in breast cancer survivors. This protocol, based on multiple studies and recommendations, involves slow, deep breathing through pursed lips, with a breathing pattern where exhalation lasts two to three times longer than inhalation.
The exercise is done three to five times per day, for 5 minutes each session, over four weeks.[3]
Immunity
A robust immune system is essential for longevity and vitality.
Slow breathing has been shown to:
- improve heart function and blood flow
- reducing stress hormones
One of the key stress hormones, cortisol, plays a complex role in immune function. It helps enhance one part of the immune system called humoral immunity, which uses antibodies to fight off infections.
However, cortisol reduces another important part called cellular immunity, where immune cells directly attack and destroy infected or cancerous cells.[4]
As we discussed in Part 1, slow deep breathing lowers cortisol levels, helping to balance immune responses.
In a study involving 27 cancer survivors, 21 of them participated in a breathing-focused workshop, where they learned specific techniques such as Sudarshan kriya and pranayama. They practiced these techniques regularly and attended weekly follow-up sessions.[5]
After 12 and 24 weeks, the study group showed a significant increase in natural killer (NK) cells, which are essential for cellular immunity and play a critical role in identifying and eliminating virus-infected and cancer cells.[6]
The study suggests that by boosting NK cell levels, these breathing techniques could potentially help reduce the likelihood of cancer recurrence or progression when studied in larger groups.
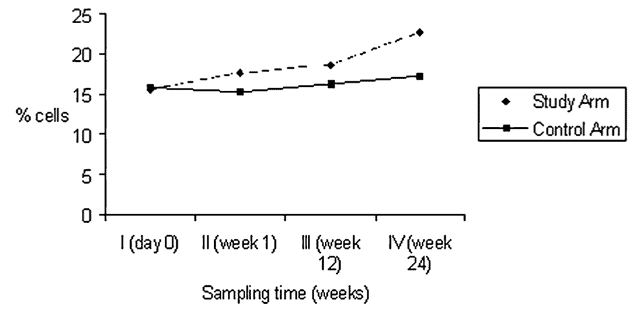
In a study that used the Nishino Breathing Method (a type of slow breathing), 21 participants attended a 90-minute exercise class.
Blood tests showed a significant increase in NK cell activity in 76% of participants. Hence this study also suggests that the immune function is enhanced by modifying breathing.[7]
Sleep
As mentioned in part one, practicing SDB for 20 minutes before bedtime can help individuals with insomnia fall asleep more easily.
In this study of 28 participants (14 with self-reported insomnia (SRI) and 14 good sleepers) two breathing intervals were tested:
- 5-second (0.2 Hz) breathing cycle
- 10-second (0.1 Hz) breathing cycle
spaced one week apart.[8]
For the slower cycle (0.1 Hz), participants:
- inhaled for three seconds
- exhaled for seven seconds
which equates to a breathing rate of six breaths per minute.
The results showed that those with insomnia:
- fell asleep faster (62% improvement in sleep onset latency compared to baseline in SRI) and
- had better sleep quality (39% reduction in number of awakenings compared to baseline in SRI)
when they practiced 0.1 Hz breathing before going to bed, but not after 0.2 Hz.
In another study involving 140 nurses, Diaphragmatic Breathing Relaxation Training (DBRT) improved sleep quality and reduced anxiety.[9]
RELATED — Introduction to Anxiety: Know what you are dealing with (Part 1)
Participants aimed for 8–10 breaths per minute for 30 minutes a day, over four weeks. Sleep quality was measured using the Pittsburgh Sleep Quality Index (PSQI), and the results were impressive:
- Global sleep quality improved by 27.82%
- Subjective sleep quality improved by 27.67%
- Sleep latency (time to fall asleep) decreased by 44.80%
- Sleep duration improved by 21.95%
- Sleep disturbances decreased by 19.08%
- Habitual sleep efficiency improved by 24.11%
- Daytime dysfunction decreased by 19.63%
RELATED — Great Sleep means Great Health: 17 Health Benefits of Good Sleep
Lastly, in a highly relevant study for today’s digital age, participants who practiced slow-paced breathing at six breaths per minute for 15 minutes before bed (using a phone app) experienced improved sleep quality compared to a control group who spent 15 minutes on social media before bed.[10]
Diaphragmatic breathing improves sleep quality and reduces anxiety
Sleep quality was measured using the PSQI and participants in the breathing group reported significantly better sleep with a 70% probability compared to someone in the control group.
In addition, their cardiac vagal activity increased, indicating that restorative processes at the cardiovascular level were enhanced during sleep.
Physical Performance
Slow breathing offers a range of benefits for athletes, enhancing both physical and mental health.[11] It can improve cardiovascular fitness, reduce stress, and support overall performance.
A study looked at an intense training session of 16 athletes, who were split into two groups.[12]
The study group – spent an hour practicing diaphragmatic breathing, focusing on their breath in a calm environment.
The control group – spent the same time sitting in an equivalent quiet place, reading magazines.
The study group showed reduced cortisol and increased melatonin, both linked to better antioxidant defenses. Oxidative stress was lower in the breathing group (11.4% lower at 2 a.m. and 17.6% lower 24 hours post-exercise) suggesting breathing exercises may improve recovery and reduce exercise-induced oxidative stress, potentially protecting them from long-term damage.
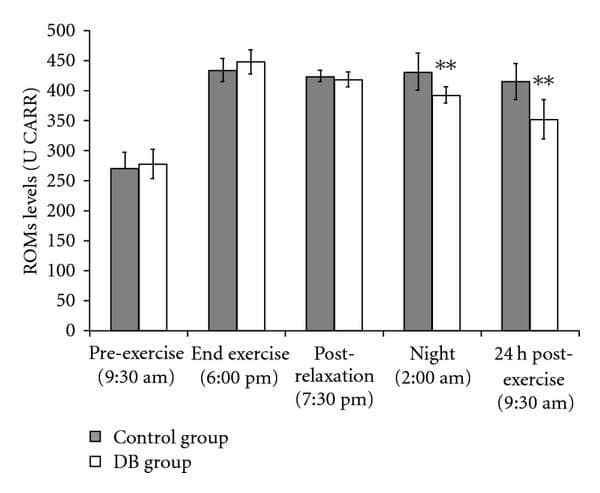
Oxidative stress (ROMs levels) were determined at different times, before and after exercise.[12]
Diaphragmatic breathing reduces cortisol and increases melatonin
Another study examined 69 elite endurance athletes and 44 healthy non-athletes, assessing their breathing patterns and lung function.[13]
Results showed that a diaphragmatic breathing pattern (using the diaphragm more fully) was linked to better lung function, with lower inspiratory reactance of 96.41% of the predicted normal value, indicating easier airflow.
By contrast, a thoracic breathing pattern (using more chest muscles) had higher inspiratory reactance, at 128.72% of the predicted value, suggesting more airway resistance.
Blood Glucose Regulation
Slow deep breathing can also play a role in managing blood sugar levels, particularly for individuals with type 2 diabetes.
A 2023 study was the first to explore the combined effects of slow deep breathing and mindfulness meditation with aerobic exercise (AT + DMM) on women with type 2 diabetes.[14]
The study randomly assigned 58 women into two groups:
- Group A performed only aerobic training (AT)
- Group B combined aerobic training with 10 minutes of diaphragmatic breathing, followed by 10 minutes of mindfulness meditation
Both groups trained three times a week for six weeks, and their serum cortisol and fasting blood glucose levels were measured at the start and end of the study.
Group B, which combined breathing and meditation with aerobic exercise, saw a 30% drop in cortisol, compared to a 20% drop in the group that only did aerobic training.
Similarly, fasting blood glucose levels dropped by 14.4% in group B, while the AT group saw a reduction of 9.9%.
Another study involving 64 nurses with type 2 diabetes examined the effects of diaphragmatic breathing exercises on blood sugar levels.[15] Half of the participants were assigned to an intervention group, where they were trained to practice diaphragmatic breathing for 20 minutes daily, along with periodic supervised sessions.
Compared to the mean fasting blood sugar (FBS) measured at the end of the first week, after nine weeks, a significant reduction was seen in the intervention group by 4.57%, while the non-intervention group experienced an increase by 10.86%.
The intervention group’s total drop in blood glucose by the 12th week was 16.9% while the control group also saw a drop of 7.5%.
Although there was no significant difference in HbA1c levels after 12 weeks, the study concluded that regular diaphragmatic breathing can have a positive effect on blood sugar control when combined with standard treatment and regular physical exercise.
Conclusion
A systematic review analyzing 58 studies with 72 total interventions found that breathing practices, when performed for a minimum of six sessions over at least a week, were significantly associated with stress-reduction benefits.[16]
This supports the idea that regular practice is essential for learning and adaptation, similar to many other skills that require consistent engagement to be effective. The results of the review are nicely summarised in the graph below.
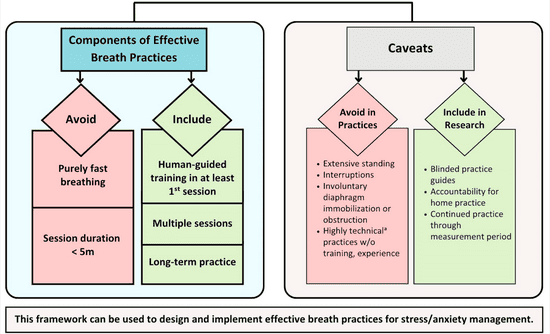
The evolutionary mismatch hypothesis suggests that the fast pace of modern life keeps our sympathetic nervous system in chronic “fight or flight” mode, contributing to insomnia, anxiety, and stress-related conditions.[17]
As we have seen so far, studies show that slow, deep breathing can counter this effect by activating the parasympathetic nervous system to support relaxation. Benefits include:
- stress reduction
- improved digestion
- enhanced sleep
- heart health
By influencing our autonomic nervous system, slow breathing offers a simple, natural approach to managing stress and enhancing overall well-being, empowering individuals to support their health effectively.
Related Questions
1. What is the effect of extending the exhale on reducing stress?
Extending exhale time activates the parasympathetic nervous system.
A study in Part 1 showed 13% reduced anxiety after 5 minutes of 4-second inhale, 6-second exhale breathing in young and older adults.[18]
2. Does alternate nostril breathing (ANB) help with anxiety?
A study focusing on alternate nostril breathing in 30 students, and the impact it had on anxiety found a positive correlation.[19]
However, due to limitations of the study, further research with a larger sample size was warranted.
3. What is hyperventilation and why does it happen
Hyperventilation is rapid, deep breathing caused by stress, anxiety, infections, or medical conditions, aiming to reduce blood carbon dioxide levels and restore pH balance.[11]
References:
(1). Jafari, H., et al. (2020). Can slow deep breathing reduce pain? An experimental study exploring mechanisms. The Journal of Pain, 21(9), 1018–1030. https://www.jpain.org/article/S1526-5900(20)30002-X/fulltext
(2) Jarrah, M. I., Hweidi, I. M., Al-Dolat, S. A., Alhawatmeh, H. N., Al-Obeisat, S. M., Hweidi, L. I., Hweidi, A. I., & Alkouri, O. A. (2022). The effect of slow deep breathing relaxation exercise on pain levels during and post chest tube removal after coronary artery bypass graft surgery. International Journal of Nursing Sciences, 9(2), 155–161. https://doi.org/10.1016/j.ijnss.2022.03.001
(3) Wang, H., Wang, T., Tan, J.-Y. (Benjamin), et al. (2022). Development and validation of an evidence-based breathing exercise intervention protocol for chronic pain management in breast cancer survivors. Pain Management
(4) Gopal, A., Mondal, S., Gandhi, A., Arora, S., & Bhattacharjee, J. (2011). Effect of integrated yoga practices on immune responses in examination stress: A preliminary study. International Journal of Yoga, 4(1), 26–32. https://doi.org/10.4103/0973-6131.78178
(5) Kochupillai, V., Kumar, P., Singh, D., Aggarwal, D., Bhardwaj, N., Bhutani, M., & Das, S. N. (2005). Effect of rhythmic breathing (Sudarshan Kriya and pranayam) on immune functions and tobacco addiction. Annals of the New York Academy of Sciences, 1056(1), 242–252.
(6) Sharrock, J. (2019). Effects of breathing techniques on immune modulation: A review. EMJ Allergy & Immunology, 4(1), 108–116. https://doi.org/10.33590/emjallergyimmunol/10311326
(7) Kimura, H., Nagao, F., Tanaka, Y., Sakai, S., Ohnishi, S. T., & Okumura, K. (2005). Beneficial effects of the Nishino breathing method on immune activity and stress level. The Journal of Alternative and Complementary Medicine, 11(2), 285–291.
(8) Tsai, H. J., Kuo, T. B. J., Lee, G. S., & Yang, C. C. H. (2014). Efficacy of paced breathing for insomnia: Enhances vagal activity and improves sleep quality. Psychophysiology, 52(2), 3–8.
(9) Liu, Y., Jiang, T. T., Shi, T. Y., Liu, Y. N., Liu, X. M., Xu, G. J., Li, F. L., Wang, Y. L., & Wu, X. Y. (2021). The effectiveness of diaphragmatic breathing relaxation training for improving sleep quality among nursing staff during the COVID-19 outbreak: A before and after study. Sleep Medicine, 78, 8–14. https://doi.org/10.1016/j.sleep.2020.12.003
(10) Laborde, S., Hosang, T., Mosley, E., & Dosseville, F. (2019). Influence of a 30-day slow-paced breathing intervention compared to social media use on subjective sleep quality and cardiac vagal activity. Journal of Clinical Medicine, 8(2), 193. https://doi.org/10.3390/jcm8020193
(11) Migliaccio, G. M., Russo, L., Maric, M., & Padulo, J. (2023). Sports performance and breathing rate: What is the connection? A narrative review on breathing strategies. Sports, 11(5), 103. https://doi.org/10.3390/sports11050103
(12) Martarelli, D., Cocchioni, M., Scuri, S., & Pompei, P. (2011). Diaphragmatic breathing reduces exercise-induced oxidative stress. Evidence-Based Complementary and Alternative Medicine, 2011, Article 932430. https://doi.org/10.1093/ecam/nep169
(13) Sikora, M., Mikołajczyk, R., Łakomy, O., et al. (2024). Influence of the breathing pattern on the pulmonary function of endurance-trained athletes. Scientific Reports, 14, Article 1113. https://doi.org/10.1038/s41598-024-51758-5
(14) Obaya, H. E., Abdeen, H. A., Salem, A. A., Shehata, M. A., Aldhahi, M. I., Muka, T., Marques-Sule, E., Taha, M. M., Gaber, M., & Atef, H. (2023). Effect of aerobic exercise, slow deep breathing and mindfulness meditation on cortisol and glucose levels in women with type 2 diabetes mellitus: a randomized controlled trial. Frontiers in physiology, 14, 1186546. https://doi.org/10.3389/fphys.2023.1186546
(15) Khanum, A., Khan, S., Kausar, S., Mukhtar, F., & Kausar, S. (2019). Effects of diaphragmatic breathing exercises on blood sugar levels in working-class females with type-2 diabetes mellitus. International Journal of Medical Research & Health Sciences, 8(1), 34–42.
(16) Bentley, T. G. K., D’Andrea-Penna, G., Rakic, M., Arce, N., LaFaille, M., Berman, R., Cooley, K., & Sprimont, P. (2023). Breathing practices for stress and anxiety reduction: Conceptual framework of implementation guidelines based on a systematic review of the published literature. Brain Sciences, 13(12), Article 1612. https://doi.org/10.3390/brainsci13121612
(17) Jerath, R., Beveridge, C., & Barnes, V. A. (2019). Self-regulation of breathing as an adjunctive treatment of insomnia. Frontiers in Psychiatry, 9, Article 780. https://doi.org/10.3389/fpsyt.2018.00780
(18) Magnon, V., Dutheil, F., & Vallet, G. T. (2021). Benefits from one session of deep and slow breathing on vagal tone and anxiety in young and older adults. Scientific Reports. https://doi.org/10.1038/s41598-021-98736-9
(19) Kamath, A., Urval, R. P., & Shenoy, A. K. (2017). Effect of alternate nostril breathing exercise on experimentally induced anxiety in healthy volunteers using the simulated public speaking model: A randomised controlled pilot study. BioMed Research International, 2017, Article 2450670. https://doi.org/10.1155/2017/2450670